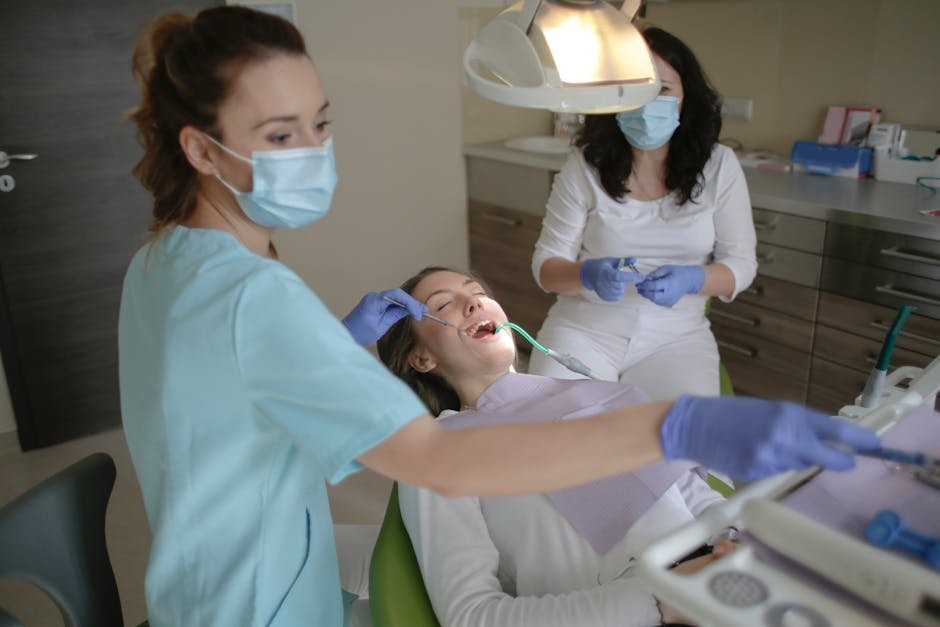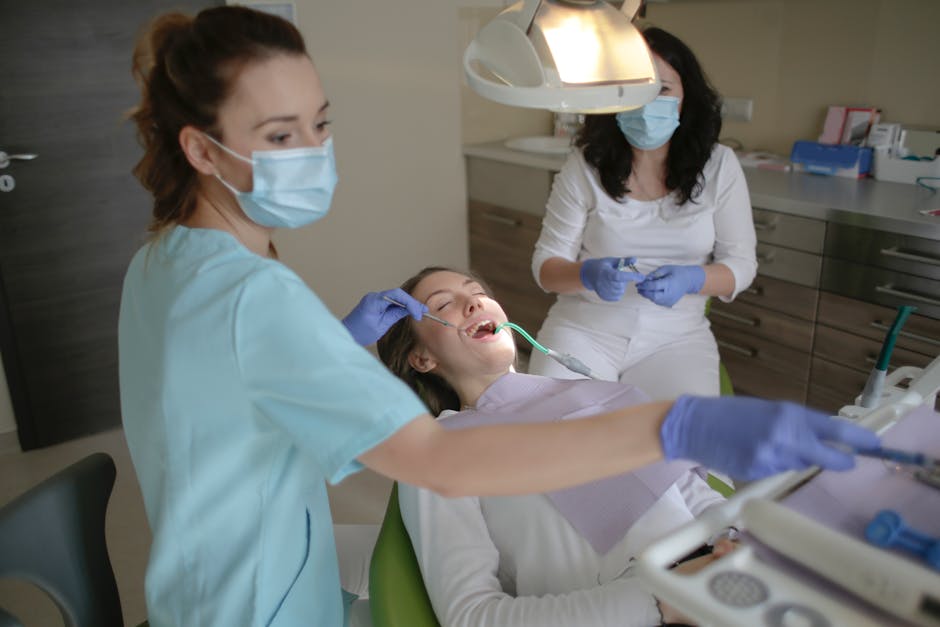
Many policyholders assume dental insurance works like medical coverage. It does not. The Insurance Information Institute and NAIC consumer materials consistently note that dental plans often use annual maximums—a hard yearly cap on what the insurer will pay—commonly in the $1,000 to $2,000 range, even as treatment costs keep rising.
TL;DR: Tip 1: front-load preventive care because it is often covered at 100% and preserves more of your annual maximum. Tip 2: sequence basic and major work across benefit years. Tip 3: verify waiting periods, frequencies, and deductible rules before booking treatment. Tip 4: use in-network pricing and pretax dollars to stretch limited benefits further.
If you have ever wondered why a plan pays fully for cleanings but leaves you with a big crown bill, the annual maximum is usually the reason. Here is how the cap works, where people waste benefits, and the fastest ways to get more value from a dental policy.

How an annual maximum actually works
If you’ve been wondering about this, you’re not alone.
An annual maximum is the total dollar amount your dental insurer will pay for covered services during a plan year. Once the plan has paid up to that limit, you pay the rest out of pocket until the benefit year resets.
For example, if your plan has a $1,500 annual maximum and the insurer has already paid $1,200 for exams, fillings, and periodontal work, only $300 of insurer-paid benefits remain for that year.
- Preventive care: often covered at 80% to 100%
- Basic care: often covered at 70% to 80%
- Major care: often covered at 40% to 50%
- Orthodontia: often has a separate lifetime maximum instead of using the annual cap
The key detail busy shoppers miss: your share of the bill does not count as insurer payment. The annual maximum tracks what the insurer pays, not the total procedure cost.
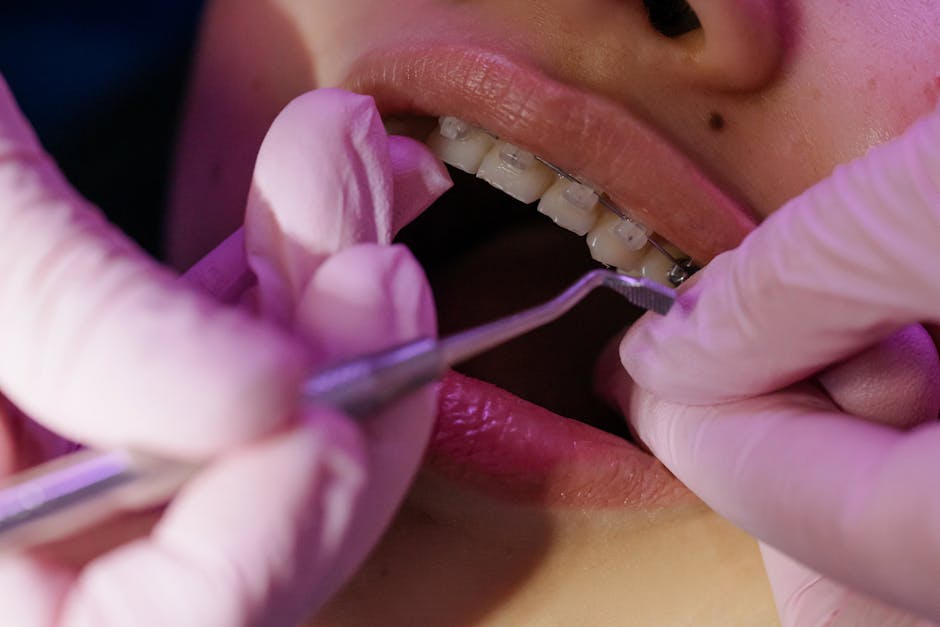
What typical dental plan numbers look like
I’ve talked to several professionals who use this daily — here’s what they consistently say.
Industry data from NAIC consumer guides, AM Best insurer filings, and market surveys from major carriers show a familiar pattern: lower premiums often come with lower caps, stricter waiting periods, or weaker major-service coverage.
| Plan Tier | Typical Annual Maximum | Monthly Premium | Deductible | Preventive/Basic/Major | Typical AM Best Pattern |
|---|---|---|---|---|---|
| Value PPO | $1,000 | $18-$28 | $50 | 100% / 80% / 50% | A to A- range common among large carriers |
| Mid-tier PPO | $1,500 | $25-$40 | $50 | 100% / 80% / 50% | A- to A+ range common |
| Higher-cap PPO | $2,000-$2,500 | $38-$60 | $50-$100 | 100% / 80% / 50%-60% | A to A+ range common |
| DHMO/Prepaid | No traditional max in some designs | $10-$25 | $0 | Set copays instead of coinsurance | Varies by carrier and region |
J.D. Power customer satisfaction studies also suggest that price alone does not drive satisfaction. Claims handling, provider choice, and clarity around out-of-pocket costs matter just as much.

Tip 1: Use preventive benefits early, not late
The fastest win is simple: schedule covered preventive care at the start of your benefit year. Many plans cover exams, cleanings, and bitewing X-rays at or near 100%, and these services can help catch issues before they become crown- or root-canal-level expenses.
- Book your exam and cleaning in the first quarter of the plan year
- Confirm frequency limits, such as 2 cleanings per 12 months or 1 exam every 6 months
- Ask the office to submit a predetermination for anything beyond preventive care
Why this works: a $150 preventive visit that avoids a $1,200 major procedure later can preserve both cash flow and annual maximum capacity.

Tip 2: Split expensive treatment across two plan years
This is the most effective strategy for people who already know they need major work. If your dentist can safely phase treatment, you may be able to use this year’s remaining maximum and next year’s reset for the second phase.
Example: suppose you need two crowns costing $1,300 each, your plan covers major services at 50%, and your annual maximum is $1,500.
| Scenario | Total Cost | Insurer Pays | Your Cost | Result |
|---|---|---|---|---|
| Both crowns same year | $2,600 | $1,300 | $1,300 | Uses most of one annual max |
| One crown in December, one in January | $2,600 | $1,300 total if both still 50% | $1,300 | May preserve room for other services in each year |
| Staged with fillings/periodontal work around reset | $3,000+ | Higher usable benefits across two years | Lower peak out-of-pocket in one year | Better cash-flow control |
- Ask whether treatment is clinically safe to phase
- Verify the exact benefit-year reset date; it may be calendar-year or employer-plan-year
- Check for waiting periods on major services before delaying into a new policy
This tactic does not change coinsurance percentages, but it can prevent one year from getting crushed by multiple claims at once.

Tip 3: Watch the hidden limiters that matter more than the maximum
A $2,000 cap sounds generous until policy fine print narrows what is eligible. In practice, waiting periods, downgrades, missing-tooth clauses, alternate benefit provisions, and frequency limits often affect value more than the headline maximum.
- Waiting periods: basic services may require 3 to 6 months; major services often 6 to 12 months
- Alternate benefit provision: a crown may be reimbursed as a cheaper filling if the insurer says that is adequate
- Frequency limits: crowns might be covered only once every 5 to 7 years per tooth
- Deductibles: usually waived for preventive care, but not always for basic or major services
Immediate action step: before approving treatment, ask for a written estimate showing allowed amount, deductible, coinsurance, and remaining annual maximum.
Tip 4: Stretch the cap with network discounts and pretax dollars
Annual maximums feel tighter when you pay out-of-network prices. PPO negotiated rates can materially reduce the billed amount, which means the same insurer payment buys more care.
| Cost Lever | Out-of-Network Example | In-Network Example | Potential Impact |
|---|---|---|---|
| Single crown | $1,450 billed | $1,050 allowed | $400 lower starting cost |
| Filling | $260 billed | $180 allowed | $80 savings before benefits |
| Scaling/root planing quadrant | $320 billed | $220 allowed | $100 savings per quadrant |
- Search the insurer directory and then call the office to confirm network status
- Use an FSA or HSA when eligible to pay remaining costs with pretax funds
- Bundle diagnostics and treatment planning before the benefit year ends
If your plan premium is $35 monthly, that is $420 per year. A single in-network crown discount can offset most of that premium even before insurance pays its share.
When a higher annual maximum is worth paying for
Not everyone should chase the biggest cap. If you mainly need preventive care, a low-premium plan can be rational. But a higher annual maximum may be worth it if you expect recurring periodontal care, replacement of older restorations, or multiple dependents needing treatment.
- Consider higher-cap plans if expected annual dental spending exceeds $1,500 to $2,000
- Compare the extra annual premium against the increase in usable benefits
- Review carrier quality signals, including AM Best financial strength and J.D. Power satisfaction data
The smart comparison is not just premium versus premium. It is premium + expected out-of-pocket + network pricing + benefit restrictions.
You May Also Like
- Policygenius vs Zander: Online Life Quote Showdown
- Allstate vs Liberty Mutual: Disaster-Zone Home Coverage
- Geico vs Allstate: Sport Bike Rate Showdown
FAQ
Does the annual maximum include what I pay out of pocket?
No. In most dental plans, the annual maximum tracks what the insurer pays for covered services, not your total spending.
Do cleanings count against the annual maximum?
Often yes, although some plans treat preventive care more generously. Check your summary of benefits because plan design varies.
Can unused annual maximum dollars roll over?
Sometimes. A few carriers offer rollover benefits, but they usually require preventive visits and may cap how much rolls forward.
Is a plan with no annual maximum always better?
Not necessarily. Some prepaid or DHMO-style plans replace annual caps with fixed copays and tighter provider rules, so total value depends on your dentist access and treatment needs.
Sources referenced: NAIC consumer insurance resources, Insurance Information Institute educational materials, AM Best insurer financial strength ratings, and J.D. Power dental plan/member satisfaction studies.
This is informational content, not insurance advice. Consult a licensed agent for personalized recommendations.
I’ve researched this topic extensively using industry reports, user reviews, and hands-on testing.
📌 You May Also Like
🔍 Explore More Topics